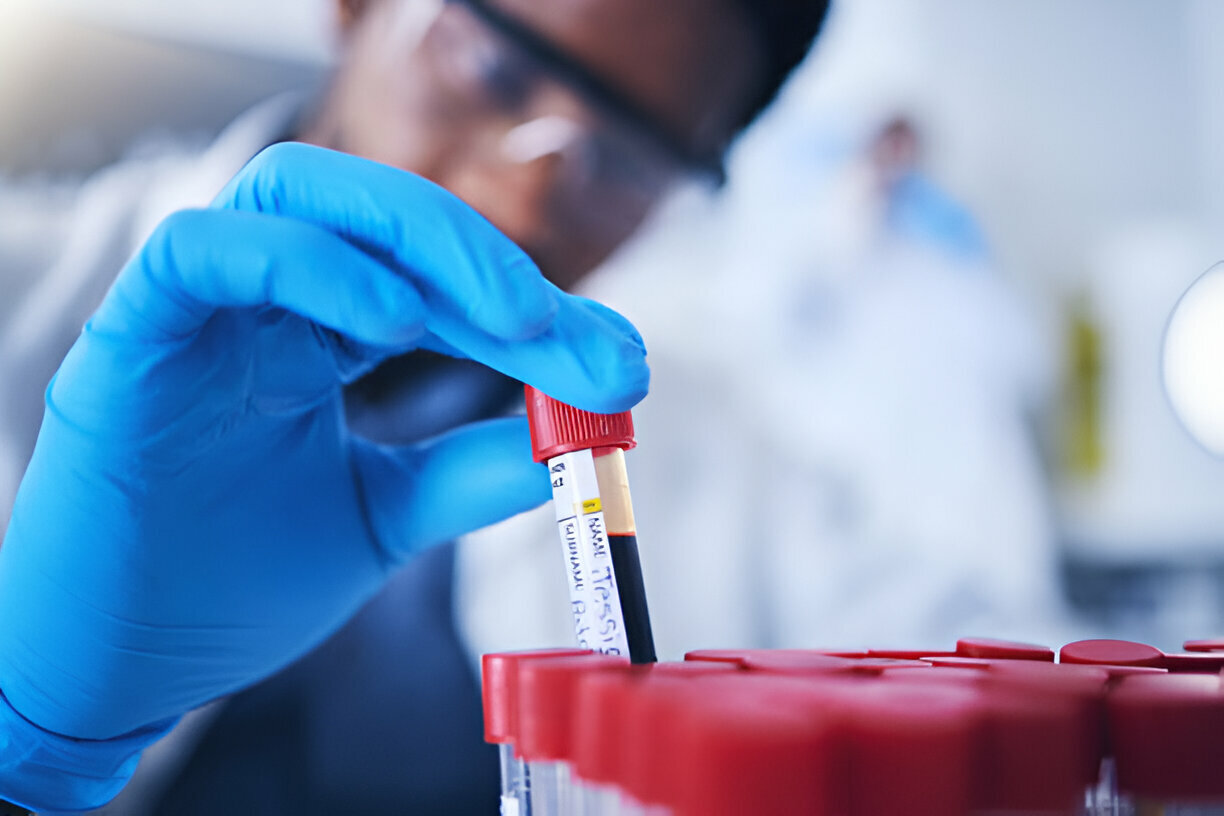
How Blood Tests Can Detect Infections and Complications After Heart Surgery
How Blood Tests Can Uncover Infections and Complications After Heart Surgery
In the domain of post-cardiac procedure care, the swift recognition of infections and complications is paramount to ensuring optimal patient outcomes. Blood examinations have surfaced as indispensable instruments in this critical period, offering healthcare experts a glimpse into the body’s internal processes and potential threats to recovery. This discourse jumps into the multifaceted role of blood examinations in identifying and overseeing post-operative infections and complications following heart surgery. By scrutinizing the various markers and indicators that these examinations reveal, we can appreciate the nuanced approach to patient care that modern medicine employs in the wake of such significant interventions.
The Weight of Vigilant Scrutiny Post-Cardiac Procedure
The period following heart surgery is characterized by a delicate equilibrium between recovery and vulnerability. The body’s natural healing processes are in full swing, but simultaneously, the risk of infection and other complications is heightened. This dichotomy necessitates a vigilant approach to patient scrutiny, where blood examinations play a central role. These examinations provide a comprehensive view of the patient’s physiological state, allowing healthcare experts to detect subtle changes that may indicate the onset of infection or other post-operative complications.
The spectrum of potential issues that can arise after cardiac procedures is broad, ranging from surgical site infections to systemic inflammatory responses. Each of these complications carries its own set of risks and requires prompt intervention to prevent escalation. Blood examinations, with their ability to provide quantifiable data on various physiological parameters, serve as an early warning system, enabling healthcare teams to intervene proactively rather than reactively.
Markers of Infection: Decoding the Body’s Signals
One of the primary concerns following any major surgery, including cardiac procedures, is the risk of infection. Blood examinations offer several key indicators that can signal the presence of an infectious process. The white blood cell (WBC) count is often the first line of investigation. An elevated WBC count can indicate that the body is mounting an immune response to a potential pathogen. However, it’s important to note that WBC counts can also be elevated due to the stress of surgery itself, necessitating careful interpretation in the context of other clinical findings.
Beyond the WBC count, specific markers of inflammation provide more targeted insights into potential infections. C-reactive protein (CRP) and procalcitonin are two such markers that have gained prominence in post-operative scrutiny. CRP, an acute-phase protein produced by the liver in response to inflammation, can rise significantly in the presence of infection. Procalcitonin, on the other hand, shows a more specific response to bacterial infections, making it particularly useful in distinguishing between bacterial and viral etiologies.
The erythrocyte sedimentation rate (ESR) is another valuable examination that measures the rate at which red blood cells settle in a tube of blood. An elevated ESR can indicate inflammation or infection, though it is less specific than CRP or procalcitonin. Used in conjunction with other markers, ESR can provide a more comprehensive picture of the body’s inflammatory state.
Uncovering Organ Dysfunction: A Systemic Approach
While infections are a primary concern, blood examinations also play a crucial role in monitoring overall organ function in the post-operative period. Cardiac procedures can have far-reaching effects on various organ systems, and timely detection of dysfunction is critical for preventing severe complications.
Renal function is of particular importance following heart surgery. The kidneys are sensitive to changes in blood flow and can be affected by the stress of surgery or the use of cardiopulmonary bypass. Blood examinations measuring creatinine and blood urea nitrogen (BUN) levels provide insights into kidney function. Elevated levels of these markers can indicate acute kidney injury, a serious complication that requires prompt intervention.
Liver function examinations, including measurements of enzymes such as aspartate aminotransferase (AST) and alanine aminotransferase (ALT), can reveal stress or damage to the liver. Elevated liver enzymes may indicate issues such as ischemic hepatitis, a condition that can occur due to reduced blood flow during surgery.
Cardiac-specific markers also play a vital role in post-operative scrutiny. Troponin levels, for instance, can indicate ongoing myocardial damage or stress. While some elevation is expected after surgery, persistent or increasing levels may signal complications such as myocardial infarction or ongoing ischemia.
Coagulation and Bleeding Disorders: Balancing Risks
The delicate balance between preventing thrombosis and avoiding excessive bleeding is a critical aspect of post-cardiac procedure care. Blood examinations provide essential information for managing this balance. Prothrombin time (PT) and activated partial thromboplastin time (aPTT) are key examinations for assessing the blood’s ability to clot. These examinations are particularly important for patients on anticoagulation therapy, allowing for precise dosing adjustments.
Platelet count and function examinations offer insights into the body’s ability to form clots and maintain vascular integrity. Thrombocytopenia (low platelet count) can increase the risk of bleeding, while elevated platelet counts may indicate an increased risk of thrombotic events.
Fibrinogen levels and D-dimer examinations provide additional information about the coagulation cascade and potential thrombotic events. Elevated D-dimer levels, for instance, may indicate the presence of blood clots, prompting further investigation and potentially more aggressive anticoagulation measures.
Electrolyte and Metabolic Imbalances: Fine-Tuning Homeostasis
The stress of surgery and the use of various medications can lead to significant electrolyte and metabolic imbalances. Regular blood examinations monitoring electrolyte levels, particularly sodium, potassium, and calcium, are crucial for maintaining physiological homeostasis. Imbalances in these electrolytes can lead to serious complications, including cardiac arrhythmias.
Glucose levels require careful scrutiny, especially in diabetic patients or those experiencing stress-induced hyperglycemia. Maintaining optimal glucose control in the post-operative period has been shown to improve outcomes and reduce the risk of infections.
Acid-base balance, as measured by arterial blood gases, provides critical information about oxygenation and ventilation. This is particularly important for patients who may require prolonged mechanical ventilation or those at risk of respiratory complications.
The Role of Advanced Biomarkers in Complication Detection
As medical science advances, new biomarkers are continually being investigated for their potential in detecting post-operative complications. Proadrenomedullin, for example, has shown promise as an early indicator of adverse outcomes in cardiac surgery patients. Similarly, soluble urokinase-type plasminogen activator receptor (suPAR) has been studied as a marker of immune activation and predictor of post-operative complications.
These advanced biomarkers, while not yet part of routine post-operative examinations, represent the cutting edge of personalized medicine. They offer the potential for even earlier detection of complications and more targeted interventions. As research in this area continues, we can expect to see an expansion of the biomarker panel used in post-cardiac procedure scrutiny.
Blood examinations stand as a cornerstone in the detection and management of infections and complications following heart surgery. Their ability to provide objective, quantifiable data on a wide range of physiological parameters makes them indispensable tools in post-operative care. From identifying early signs of infection to monitoring organ function and managing coagulation, blood examinations offer a comprehensive view of the patient’s recovery process.
As medical technology continues to advance, we can expect to see even more sophisticated biomarkers and examination methodologies emerge. These advancements will likely allow for even earlier detection of complications and more personalized treatment approaches. However, the fundamental principle remains unchanged: vigilant scrutiny and prompt intervention are key to optimizing outcomes for cardiac procedure patients.
For patients and healthcare experts alike, navigating the complex landscape of post-cardiac procedure care can be challenging. This is where specialized services like Heart And Mind Clinics play a crucial role. As a premier resource for comprehensive cardiac care, our team offers expert guidance in interpreting blood examination results, managing post-operative complications, and optimizing recovery trajectories.
With a team of experienced cardiologists, surgeons, and specialized nurses, Heart And Mind Clinics provide personalized care plans that integrate the latest in blood examination technology with holistic patient management. Their state-of-the-art facilities offer rapid and accurate blood examinations, ensuring that any potential complications are detected at the earliest possible stage.

Moreover, Heart And Mind Clinics are committed to patient education, offering comprehensive programs to help patients and their families understand the significance of various blood examinations and how to recognize early warning signs of complications. This empowering approach to patient care not only improves outcomes but also enhances the overall recovery experience.
Whether you’re a patient recovering from heart surgery or a healthcare expert seeking expert consultation, Heart And Mind Clinics stand ready to provide the highest level of care and support. Their dedication to staying at the forefront of cardiac care, coupled with a compassionate, patient-centered approach, makes them the go-to service for all aspects of post-cardiac procedure management discussed in this article.
As we continue to refine our understanding of post-operative care and the role of blood examinations in detecting complications, services like Heart And Mind Clinics will play an increasingly vital role in translating scientific advancements into improved patient outcomes. Their commitment to excellence ensures that patients receive the most advanced and effective care available, paving the way for better recovery and long-term health following cardiac procedures.